CAPD: Statement for the Record, U.S. Senate Committee on Health, Education, Labor and Pensions
The Coalition for Affordable Prescription Drugs (CAPD) appreciates the opportunity to submit the following statement for the record.
The Coalition for Affordable Prescription Drugs (CAPD) represents a diverse group of large employers, labor unions, health plans, public sector employees and retirees, and other stakeholders who partner with pharmacy benefit managers (PBMs) to help manage costs so that they can continue to offer affordable, accessible health and drug benefit coverage to their employees and members.
We appreciate Chairman Alexander’s scheduling of this critically important hearing today, because prescription drug prices are increasing at an unsustainable rate, to the detriment of patients, employers, taxpayers, and our health care system, and recent research shows that an overwhelming majority of Americans believe that lowering drug prices is an “extremely” or “very” important priority for Congress.1
An important fact, and one that is often overlooked in the debate over high drug prices, is this: drug manufacturers — and drug manufacturers alone — set the price for prescription medicines.
We are fortunate to live in a time of unprecedented medical breakthroughs. Manufacturers are developing treatments and cures for diseases like Hepatitis C that improve and extend the lives of patients. We all want patients to have access to these medicines, but the innovative power of these medicines is rendered moot when patients are unable to afford them.
At an event this month sponsored by our coalition, former CMS Administrator Thomas Scully emphasized that while manufacturers must be given a fair return on investment, drug companies should not be able to simply “invent a price,” which he said is what is happening now. He stressed that prices should be aligned with value and cost.
The most impactful change to make medicines more affordable for patients would be for manufacturers to set a responsible price. Yet, manufacturers’ prices continue to rise2, increasing by more than nine percent in 2016 alone, following double-digit increases every year since 2012.
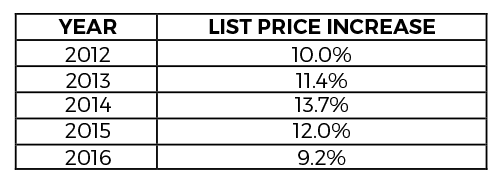
It is important to realize that the prices set by manufacturers – which are growing by double digits annually – are the starting point. Pharmacy benefit managers (PBMs) use their size and scale to negotiate the lowest net price for prescriptions and drive down costs on behalf of employers, unions and other health care purchasers, if the starting point is unreasonably high, the effects ripple throughout the system.
Pharmacy benefit managers have managed to keep the net prices that their clients pay steady, increasing only 3.5 percent the same year3 that manufacturer list prices rose 9.2 percent. That difference represents savings for PBM clients – the employers, unions, retirement plans and government programs that provide health care coverage to 266 million Americans4. More than 90 percent of these savings are passed on to the employers and unions, and are used to lower out of pocket costs and premiums for employees and members.
In addition to delivering savings through negotiations with drug manufacturers, PBMs support better health outcomes and help reduce health care costs through multiple strategies. Deep clinical expertise helps ensure the safest, most effective and affordable medications are dispensed, which in many cases is a generic drug. Patient-focused tools and programs also help to improve medication adherence, which is critically important to the one out of every two Americans with a chronic disease.
Patients’ out of pocket costs are one of the most significant barriers to medication adherence. The reality is this: if manufacturers set prices at more reasonable levels – and increased them only at a sustainable rate – potentially life-saving medicines would be more accessible to the patients that need them. We know this because pharmacy is a major driver of cost in the health care system, and when those prices are increased at an unsustainable rate, sometimes unexpectedly on older medicines5, patient co-pays and premiums follow suit.
Fortunately, as the drug price debate continues, the focus is increasingly turning to understanding the prices that drug manufacturers are setting. This was evident at the first hearing this Committee held on drug prices in June. As Gerard Anderson, Professor of Medicine at Johns Hopkins University School of Medicine, testified6 at the hearing, “Many people have argued that the list price is irrelevant because few entities actually pay the list price. However, the list price is often used to determine the amount of cost sharing that many patients will pay. Since the list price is the only price that is publicly announced, it becomes the basis for many cost‐sharing agreements. Thus, patients are harmed when the list price goes up.”
Ensuring greater access and affordability will also depend on fostering greater competition. Facilitating faster reviews of generics and biosimilars, identifying off-patent drugs with little or no generic competition, and ending anti-competitive practices that keep safe, effective alternatives off the market are also key to managing rising drug costs for patients. A competitive environment ensures that PBMs can effectively negotiate on behalf of their partners, ensuring access to needed medications and, at the same time, bending the cost curve of rising drug prices.
CAPD is grateful for the opportunity to submit this testimony and eager to work with stakeholders to find new ideas and build on existing strategies to help drive progress for employers, employees, retirees, taxpayers – and for America’s future.
1 http://www.politico.com/story/2017/09/25/politico-harvard-poll-congress-should-focus-on-reducing-drug-prices-243109
2 http://www.imshealth.com/en/thought-leadership/quintilesims-institute/reports/medicines-use-and-spending-in-the-us-review-of-2016-outlook-to-2021
3 http://www.imshealth.com/en/thought-leadership/quintilesims-institute/reports/medicines-use-and-spending-in-the-us-review-of-2016-outlook-to-2021
4 https://www.pcmanet.org/wp-content/uploads/2016/11/ROI-on-PBM-Services-FINAL.pdf
5 https://khn.org/news/climbing-cost-of-decades-old-drugs-threatens-to-break-medicaid-bank/
6 https://www.help.senate.gov/imo/media/doc/Anderson4.pdf
